
Optometric vision therapy develops visual skills which are inadequate for an individual’s needs either due to delayed development or trauma. While vision skills must be integrated to become automatic and improve function, they are divided into two categories.
• Ocular motor skills: tracking across a page of print while reading, maintaining fixation while studying an object of interest, converging your eyes to look at something that is near to you, following a ball, looking back-and-forth to copy, and focusing.
• Visual information processing skills: judging distance, size, and speed; figure-ground (crowding); visual memory and visualization; speed of processing; filtering extraneous information to maintain visual attention; motor planning; and scanning.
Vision therapy always involves the integration of skills from both areas. Reading is an example of the importance of this integration as are the visual motor skills of writing and drawing. The conditions treated by vision therapy are strabismus, amblyopia, convergence insufficiency and other eye teaming problems when the eyes are usually aligned, learning-related vision problems, and visual problems associated with post-concussion syndrome
Every patient is unique. Therapy sessions in the office are programmed by Dr. Williams and implemented by trained optometric vision therapists. Irene Anderson and Sarah McDowell are both Certified Optometrist Vision Therapists (COVT) through the College of Optometrists in Vision Development. Dr. Williams is a Fellow in COVD (FCOVD). COVD is the international certification organization for vision therapy. Dr. Williams is a past president of COVD and was the chairperson of continuing education for 18 years.

Amblyopia describes reduced visual function in an otherwise healthy eye. Most of the early research on neuroplasticity in the brain has been done with amblyopia. Vision will not develop properly when an eye is not given appropriate developmental experiences. This occurs when an eye is turned and is ignored by the brain to avoid double vision and confusion. It also occurs when the image from an eye is consistently out of focus as happens when one eye is much more farsighted than the other or both eyes have high degrees of astigmatism.
Amblyopia is described by the best visual acuity obtainable with glasses, but the visual detriment involves much more than acuity. An eye with amblyopia does not track as well, it processes information more slowly, it perceives objects as running together, and does not see sequences in the correct order. It is the most common cause of blindness in children and young adults. Recent research has changed the treatment of amblyopia with higher rates of success. A child with amblyopia rarely realizes that they have a problem. It is what they are used to.

Convergence insufficiency is the most common of the disorders in which the eyes do not team and focus together automatically. These problems are common in children and adults. They are assessed through a combination of signs, symptoms, and testing. (See the Convergence Insufficiency Symptom Survey.) These conditions often go unrecognized because the signs and symptoms have a variety of possible causes and are usually not assessed in routine eye examinations. Adults may just accept their discomfort and difficulties as normal; something else we have to live with. In children these visual problems are often mis-attributed to attention deficit disorder, learning disabilities, or laziness.
The demands for hours of concentrated visual activities within arm’s reach continues to increase. Young children are expected to read one year earlier than their parents were expected to read. Print size gets small and pages get crowded before many children have the visual skills to handle this visual and cognitive load. Children are also involved with staring at illuminated screens for hours a day starting at a young age. This causes eyestrain for many of them (but they may persist due to their engagement in what they are doing). It also reduces the type of play that children did a generation or two ago which are instrumental in the development of visual (and other) skills.
Most adults spend time looking at illuminated screens. (See computer use and eyestrain). This is one of many examples of what we do in the 21st century which is a challenge to how we have adapted through evolution. Our vision adapted to help us to survive and navigate, not to stare at small print. Across the developed world, more people are becoming increasingly nearsighted. Researchers have not determined all of the contributing factors, but changes in our lifestyle are a factor.
Convergence insufficiency and related problems can be treated with glasses, vision therapy, or a combination of treatments. Treatment is effective in children and adults. Modifications in what people do and how they do it are frequently part of the treatment. Inadequate rest is common in all age groups and makes these problems worse. These problems are common in people who have had a head injury and now have post-concussion syndrome.

People who have had a head injury may experience visual problems as part of their post-concussion syndrome. These include sensitivity to light, difficulty focusing, motion sickness, headaches due to eyestrain, inability to read, and being visually overwhelmed by busy environments such as stores.
The initial treatment for head injuries, after imaging studies, is rest. The brain has an amazing ability to heal itself with rest, but rest for the brain is relative and not always easy for the individual to accomplish. Everything that we do, including sitting, thinking, and worrying, adds to brain activity. After a brain has been injured, it is extremely vulnerable to being overloaded. The symptoms caused by overload and the time it takes to recover are exaggerated when the brain has been injured. Prior to a head injury, pushing through discomfort may be a reasonable choice, but this is no longer an effective strategy. Since it does not take much to become overloaded, the person and family are often blindsided when it happens.
Controlling the amount of light, contrast, and glare are important to avoid over-stimulation. This is managed by modifying the environment, using various densities and colors of tinted lenses, and sometimes through partially covering one or both eyeglass lenses to reduce stimulation.
• The focal system is what comes to mind when we think of vision. We are conscious of seeing what is around us. We see detail. We see color. We recognize people and other objects in our environment. We associate objects with their names. We read.
• The ambient system works in the background and is just as important as the focal system, but we are not aware of it until we experience a sudden problem. Some children have difficulties with their ambient vision but do not realize it because it has always been that way. Our tests for ambient vision are not as precise at this time as those that we have to assess focal vision. Ambient vision guides most of our eye movements. Ambient vision allows us to handle large amounts of visual stimulation and helps us to filter out the distractions from what we want to focus on. Ambient vision coordinates with the rest of our body, including our inner ears and the receptors in our neck to enable us to move and have objects move around us without causing dizziness and disorientation. Ambient vision is a critical component of our balance system.
A combination of modifications to the environment, careful selection of activities, limiting the duration of activities, and prescribing lenses, tints, and vision therapy are the tools to rehabilitate the visual system. It is often impossible to predict the degree and rate of recovery after head injuries. This is disappointing, but accepting that recovery will be step-by-step and focusing on the recovery is very important. The stress of continuously being frustrated at the rate of rehabilitation is an overload which can stall recovery.
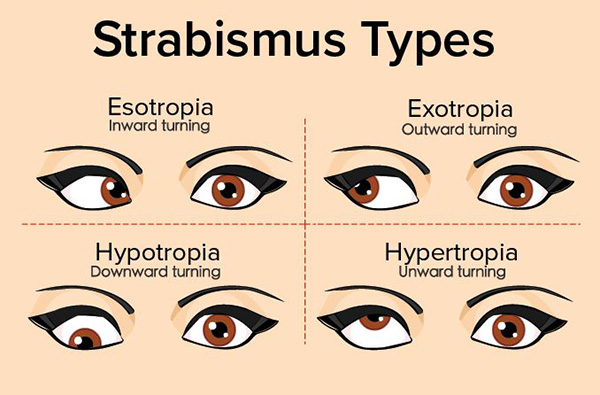
Strabismus describes when an individual’s eyes do not align. The misalignment may be constant or intermittent. In most cases, this is not due to a faulty eye muscle, nerve, or mechanical restriction but rather due to poor neuromuscular coordination, this can often be improved through vision therapy. Even when there is a physical reason for the eye turn, vision therapy can often improve cosmetics and function. Children’s eyes tend to wander independently for the first month or so after they are born similar to the random movements of their arms and legs. This should not occur after the first three months. If an eye is misaligned constantly from an early age, the vision in that eye will be ignored by the brain to reduce confusion and the visual function of that eye will not develop properly which is known as amblyopia.